Mayo Clinic Pilot Trial: Detection of Gastrointestinal Bleeding Using the Pulse Flowmeter
A Prospective Pilot Study — Mayo Foundation for Medical Education and Research, Rochester, MN
Authors: Hadi Khaled Abou Zeid, Yara Salameh, Elizabeth Lemke, Manik Aggarwal, Andrew C. Storm
Department of Gastroenterology and Hepatology, Mayo Foundation for Medical Education and Research, Rochester, MN
Wake Forest University School of Medicine, Winston-Salem, NC
Background
Accurate detection of occult gastrointestinal bleeding remains a significant clinical challenge. Conventional hemodynamic monitoring — heart rate and blood pressure — often fails to identify active bleeding until a patient has lost approximately 40% of blood volume and is approaching cardiovascular collapse. The MGI Pulse Flowmeter (PFM) introduces novel hemodynamic parameters — Pulse Volume (PV), Pulse Flow (PF), and the Compensated Shock Index (CSI = PV ÷ Heart Rate) — to assess peripheral perfusion status and identify compensated shock before conventional vital signs are affected.
This prospective pilot study evaluated the feasibility and clinical utility of the PFM in identifying GI bleeding in patients undergoing endoscopy for suspected GI hemorrhage.
Methods
Thirteen patients were enrolled; one was disenrolled, leaving 12 evaluable subjects. Continuous monitoring captured Pulse Volume, Pulse Flow, Compensated Shock Index (CSI), Heart Rate, and Baseline Impedance (Ro) before and after endoscopy using the Advanced Pulse Flowmeter device. Physiological parameters were averaged over five-minute intervals. Device performance, physiological validity, and ability to detect occult bleeding were assessed.
Results
The PFM functioned normally in a busy clinical environment. All recorded data were within expected physiological ranges.
Active bleeding prediction was correct in 12 of 12 patients (100%).
- The two patients with progressive CSI decline were found to have active bleeding confirmed at endoscopy.
- Patients with stable CSI did not have active bleeding.
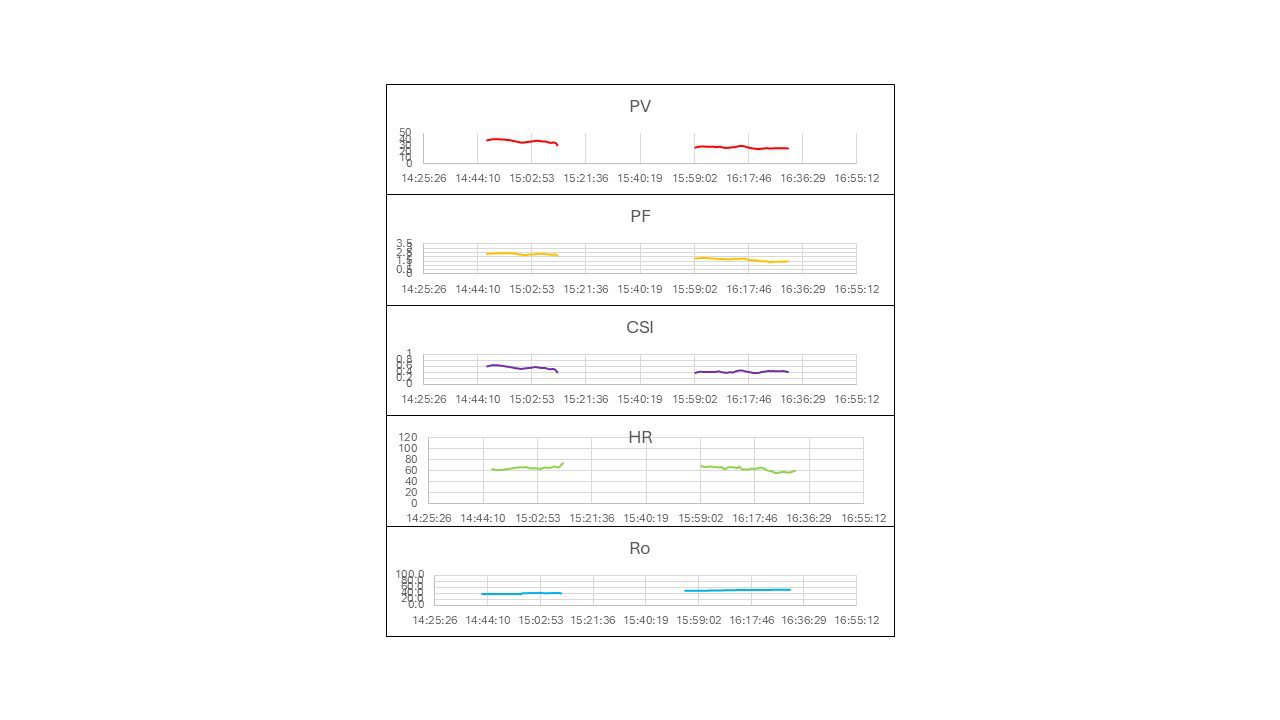
- In one particularly notable case, pre-endoscopy declines in Pulse Volume and Pulse Flow with characteristic CSI behavior led to a prediction of active bleeding — confirmed endoscopically — despite completely normal conventional vital signs throughout monitoring.
Conclusions
The MGI Pulse Flowmeter accurately provided real-time perfusion monitoring and occult bleeding detection in this prospective pilot trial. Recorded metrics (PV, PF, CSI) aligned in all 12 cases with endoscopic evidence of active bleeding and provided physiological signal beyond routine vital signs. The investigators concluded that larger-scale prospective trials are warranted to validate the PFM as a novel tool for hemodynamic assessment in gastrointestinal bleeding.
Clinical Significance
This trial demonstrates that the PFM can detect active GI bleeding in patients who appear hemodynamically stable by conventional measures. This capability has significant implications for triage decisions, timing of intervention, and patient safety in emergency and inpatient GI settings.
This study was conducted at the Mayo Foundation for Medical Education and Research, Rochester, Minnesota. MGI Medical provided the Advanced Pulse Flowmeter device used in this investigation.
Figure 1. Representative hemodynamic metrics from the Advanced Pulse Flowmeter showing Pulse Volume (PV), Pulse Flow (PF), Compensated Shock Index (CSI), Heart Rate (HR), and Baseline Impedance (Ro) over time. Despite normal vital signs, this patient showed a 22% decrease in PV, a 9% decrease in PF, a 10% increase in HR, and a 35% decrease in CSI prior to endoscopy — predicting active bleeding that was confirmed endoscopically.